By: Sarah Pember
October is Health Literacy Month, a time to promote effective communication to avoid misinterpretation in health care, promotion, and education. People of all ages need to be able understand health information to make the best decisions for themselves and their loved ones. Health literacy skills involve finding health information and services, communicating needs and preferences, processing and understanding the given choices and associated consequences, and, ultimately, deciding which choices to make and acting upon them.
There are three types of health literacy:
Improved health literacy is linked to improved health outcome, because of higher patient satisfaction, appropriate utilization of medical services, more effective treatments, less provider frustration, and overall lower economic burden.
October is Health Literacy Month, a time to promote effective communication to avoid misinterpretation in health care, promotion, and education. People of all ages need to be able understand health information to make the best decisions for themselves and their loved ones. Health literacy skills involve finding health information and services, communicating needs and preferences, processing and understanding the given choices and associated consequences, and, ultimately, deciding which choices to make and acting upon them.
There are three types of health literacy:
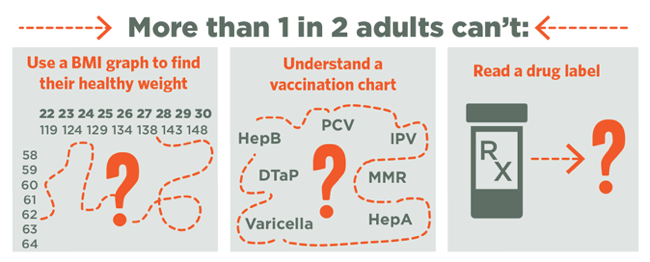
- Functional Literacy: Basic reading and writing skills that enable consumers to follow health messages (i.e. Read prescription bottles, literature in physician/dentist offices, nutrition panels, health guidelines)
- Interactive literacy: Advanced literacy, cognitive, and interpersonal skills that enable consumers to navigate the healthcare system
- Critical literacy: Critical thinking skills that enable consumers to evaluate information for credibility and quality, analyze relative health risks, and interpret health test results
Improved health literacy is linked to improved health outcome, because of higher patient satisfaction, appropriate utilization of medical services, more effective treatments, less provider frustration, and overall lower economic burden.
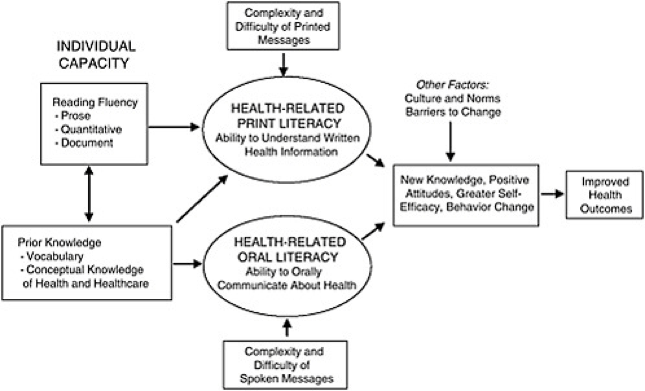
Conceptual Model of the Relationships
Between Individual Capacities, Health Literacy,
& Health Outcomes (Baker, 2006)
Culture is a key influence on health literacy and effective communication between health provider and patient, or program leaders and participants. Cultural awareness—of tradition, custom, appropriate modes of communication—can improve the overall translation of health information. It is important to remember however, that cultural awareness is more than just language. For example, in providing dietary recommendations, it is one thing to translate a webpage or document into Spanish, but entirely more beneficial if that resource also includes foods common to a Latino culture, such as tortillas and nopales.
As a patient, you must ask questions: What is my main problem? What do I need to do? Why is it important for me to do this?
As a provider of health care or information, you can improve communication by using the following strategies:
Resources and References:
Between Individual Capacities, Health Literacy,
& Health Outcomes (Baker, 2006)
Culture is a key influence on health literacy and effective communication between health provider and patient, or program leaders and participants. Cultural awareness—of tradition, custom, appropriate modes of communication—can improve the overall translation of health information. It is important to remember however, that cultural awareness is more than just language. For example, in providing dietary recommendations, it is one thing to translate a webpage or document into Spanish, but entirely more beneficial if that resource also includes foods common to a Latino culture, such as tortillas and nopales.
As a patient, you must ask questions: What is my main problem? What do I need to do? Why is it important for me to do this?
As a provider of health care or information, you can improve communication by using the following strategies:
- Slow down when speaking
- Use plain language without technical/professional jargon
- Limit the amount of information provided, and repeat it
- Show or provide pictures
- Use teach-back or show-me techniques
- Create a shame-free environment
Resources and References:
- Baker, D. W. (2006). The meaning and the measure of health literacy.Journal of general internal medicine, 21(8), 878-883.
- Centers for Disease Control and Prevention. (2016) . Health Literacy. Retrieved from http://www.cdc.gov/healthliteracy/
- Osborne, H. (2016) Health Literacy Month. Retrieved from http://www.healthliteracymonth.org/
 RSS Feed
RSS Feed
